Lymphatic drainage massage
Edit Column Revitalise Your Body And Mind: The Ultimate Guide To Lymphatic Drainage Massage Edit Column Revitalise Your Body And Mind: The Ultimate Guide To Lymphatic Drainage Massage Edit Column…
Edit Column Revitalise Your Body And Mind: The Ultimate Guide To Lymphatic Drainage Massage Edit Column Revitalise Your Body And Mind: The Ultimate Guide To Lymphatic Drainage Massage Edit Column…
Attention! Neck pain sufferers, listen up! Do you know that your neck is one of the most complex and delicate parts of your body? And, there are several factors that…
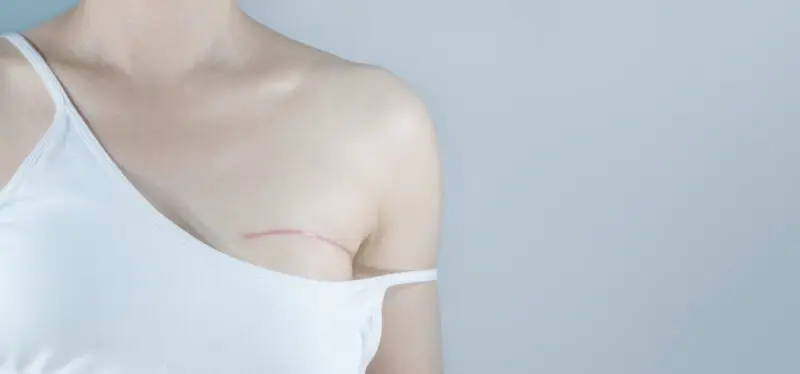
Scars are a natural part of the healing process that occur after injury or surgery. When the skin is damaged, the body produces collagen to repair the wound. This can…
Question… Which is the largest organ in the human body? A lot of people think the answer is the brain, lungs or liver when asked this question. When in fact,…
It’s morning, and the alarm clock has just told you it’s time to get out of bed. Another few minutes won’t hurt. You check your emails, social media sites, and…
Both Acupuncture and Dry Needling involve the insertion of a filiform stainless-steel needle through the skin to alleviate pain, but are they different and if so, how? Let's begin by…
Have you ever been told you are flat-footed? Or have you noticed that the arches in your feet are not quite the same as others? Although we are all a…
It has been and continues to be, uncertain times for many of us as the COVID-19 pandemic continues to sweep across the globe. Lockdown has meant many of us have…
A very common question we get asked at Completely Aligned is “Do I need to wear a brace to help with my injury?” Well this is very much a ‘depends’…
Hello readers! This month’s blog topic is one that millions of Australians (and billions around the world) can relate to. Have you ever had a headache? We’d be surprised if…